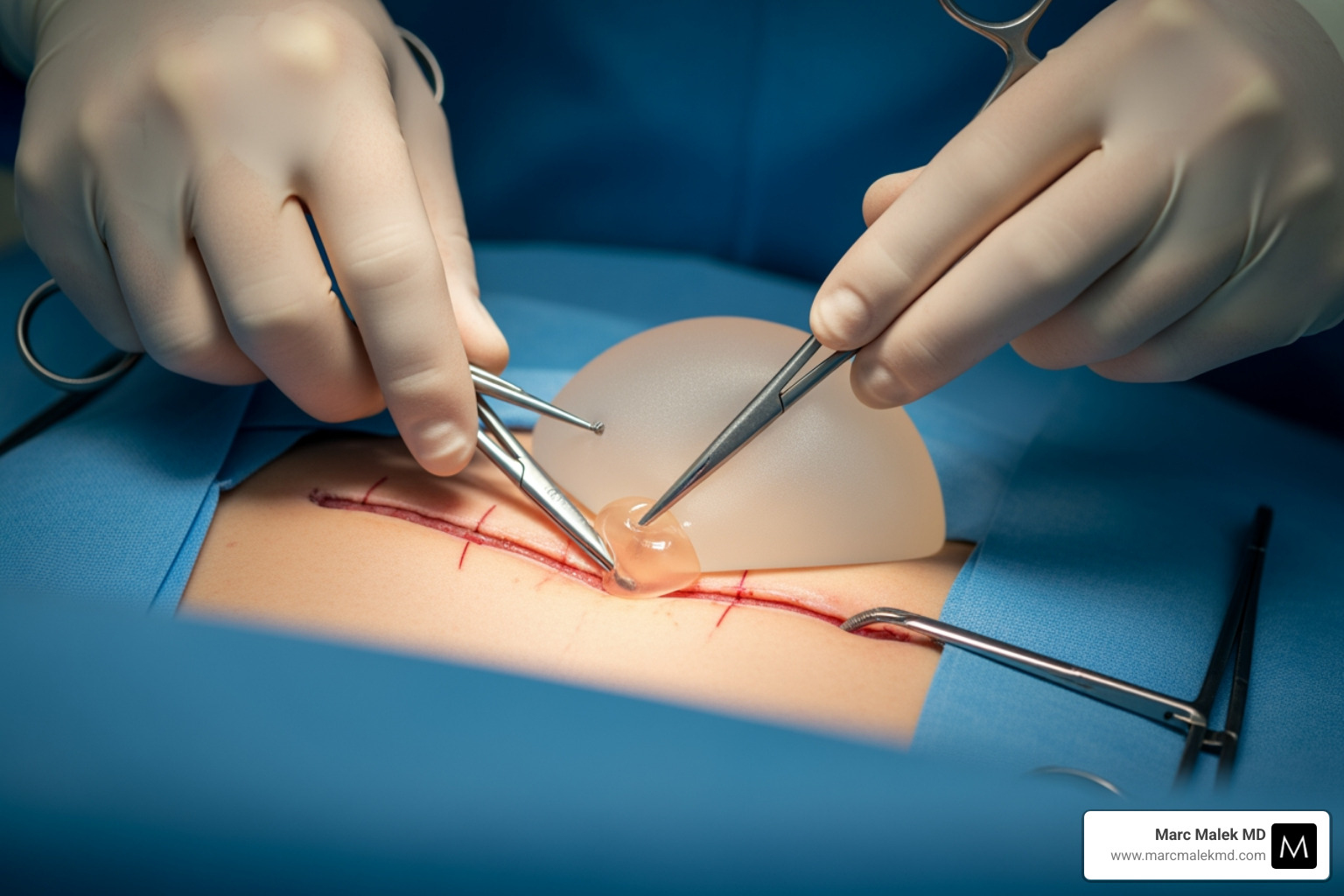
Understanding Your Path to Silicone Implant Removal
Silicone implant removal is a surgical procedure to take out breast implants and, when necessary, the surrounding scar tissue capsule. Whether you’re experiencing complications, noticing changes in your body, or simply ready for a new chapter, understanding this process is the first step toward making the right decision for your health and confidence.
Quick Guide: Why Women Choose Implant Removal
Common Reasons:
- Implant aging – Implants are not lifetime devices; replacement recommended every 10-15 years
- Rupture or leakage – Silicone gel can leak silently, requiring MRI for detection
- Capsular contracture – Hardening of scar tissue around the implant causing pain
- Personal preference – Body changes from pregnancy, weight shifts, or lifestyle
- Health concerns – Systemic symptoms or rare conditions like BIA-ALCL
The Process:
- Consultation with a board-certified plastic surgeon
- Pre-operative imaging (MRI or ultrasound) if rupture suspected
- Surgery under general anesthesia (typically 1-2 hours)
- Recovery period of 1-2 weeks for initial healing, up to 6 weeks for full recovery
- Optional concurrent procedures like breast lift or fat grafting
Breast implants are not designed to last forever. Research shows that rupture rates reach 15% at the 10-year mark. Many women go through life changes—pregnancies, weight fluctuations, evolving aesthetic preferences—that make their once-perfect implants feel wrong for their current body and lifestyle.
You might be here because your implants no longer feel right, or because your doctor detected a problem. Maybe you’re experiencing unexplained symptoms you suspect might be related to your implants. Or perhaps you’re simply ready to accept your natural shape again.
Whatever brings you to this decision, you’re not alone. The journey from consideration to recovery involves understanding your options, finding the right surgeon, and planning for the aesthetic outcome you want. This guide walks you through each step, from recognizing why removal might be right for you to understanding what your breasts will look like afterward.
Why Consider Explant Surgery? From Personal Choice to Medical Necessity
Choosing to undergo silicone implant removal is a deeply personal decision, often driven by a mix of evolving aesthetic preferences, lifestyle changes, or, crucially, medical necessity. We understand that this is a significant step, and we’re here to guide you through why someone might need this procedure.
Breast implants, whether saline or silicone, are not lifelong devices. The American Society of Plastic Surgeons and many medical professionals recommend that implants be exchanged or removed approximately every 10 to 15 years. This isn’t just a suggestion; it’s a recognition that implants age, and with age, the risk of complications increases. For instance, if you had silicone implants placed before 1989, it’s highly likely they have ruptured due to aging, and we recommend discussing removal with a surgeon.
Beyond the recommended timeline, many women simply experience a change of heart. What felt right in one phase of life might not align with another. Pregnancy, breastfeeding, significant weight fluctuations, or even a shift in personal style can lead to a desire for a different breast aesthetic. You might find your implants no longer fit your body’s size or shape, or perhaps you’re seeking a more natural look.
However, often the decision for silicone implant removal stems from medical reasons. These can range from common complications to more serious health concerns that necessitate surgical intervention.
To properly assess the integrity of your implants and identify potential complications, diagnostic methods are crucial. Magnetic Resonance Imaging (MRI) is considered the most sensitive test for detecting implant integrity, especially for silicone implants, which can rupture silently without obvious symptoms. Ultrasound can also be used for detection. If a rupture is suspected, mammography should generally be avoided until the issue is clarified.
Understanding the Reasons for Silicone Implant Removal
The aging process of implants is a primary driver for removal. As mentioned, implants are not meant to last a lifetime. After 10 years, the risk of rupture significantly increases, with studies reporting a 15% rupture rate at this mark.
A key distinction lies between a ruptured saline implant and a ruptured silicone implant, and how this affects removal. If a saline implant ruptures, the saline solution is harmlessly absorbed by the body, and the breast will visibly deflate. While not a health risk, it’s certainly a cosmetic concern.
In contrast, a ruptured silicone implant removal is a more complex matter. Silicone gel, if it leaks, can remain contained within the scar tissue capsule (intracapsular rupture) or, more concerningly, extrude beyond it (extracapsular rupture) into surrounding breast or chest wall tissues. This can lead to scar formation, making the breast feel lumpy, hard, or cause persistent pain. Because silicone rupture can be “silent” – meaning it occurs without noticeable symptoms – regular monitoring with MRI is vital. If a silicone implant is ruptured, we generally recommend prompt removal to prevent further gel migration and potential complications.
Another common reason for silicone implant removal is capsular contracture. This occurs when the fibrous capsule of scar tissue that naturally forms around any implant tightens and squeezes the implant. This can cause the breast to become firm, hard, misshapen, and often painful. The severity of capsular contracture is often graded using the Baker scale, from I (soft, normal appearance) to IV (hard, painful, distorted). A Baker Class IV contracture with severe pain is a common medical indication for removal.
For more detailed information on your various breast surgery options, including revision and removal, please explore our resources at More info about your breast surgery options.
Systemic Symptoms and Serious Health Concerns
Beyond localized complications, some individuals with breast implants report a range of systemic symptoms they attribute to their implants. This constellation of symptoms is often referred to as Breast Implant Illness (BII). While the medical community is still actively researching BII, and direct causation is not yet definitively proven, patients report symptoms such as joint pain, muscle aches, chronic fatigue, confusion (“brain fog”), hair loss, skin rashes, and even autoimmune-like conditions. We recognize and validate these patient experiences. A joint safety advisory from leading aesthetic surgery societies notes that patients often report significant symptom improvement after implant removal, even without full capsulectomy. If you are experiencing such symptoms, we encourage a thorough medical evaluation to rule out other causes before considering silicone implant removal.
A more serious, though rare, concern is Breast Implant-Associated Anaplastic Large Cell Lymphoma (BIA-ALCL). This is a rare type of non-Hodgkin’s lymphoma that can develop in the fluid or scar tissue capsule surrounding breast implants, particularly textured silicone implants. It is not breast cancer, but an immune system cancer. Symptoms often include persistent swelling, pain, or a mass around the implant. The FDA has issued safety communications regarding BIA-ALCL, and in some cases, certain textured implants have been recalled. While the risk is very low (estimated at 0.3% per 100,000 women per year), if BIA-ALCL is diagnosed, the recommended treatment is surgical removal of the implant and the entire surrounding capsule.
Additionally, recent FDA communications have highlighted reports of Squamous Cell Carcinoma (SCC) and various other lymphomas found in the capsule around breast implants. While these are also rare, they underscore the importance of proper diagnostic evaluation and surgical removal of the capsule when implants are explanted due to medical concerns.
Your Guide to the Silicone Implant Removal Procedure
Once the decision for silicone implant removal has been made, understanding the procedural journey can help alleviate anxieties and set realistic expectations. From your initial consultation to the post-operative testing, we’ll walk you through what to expect.
During your pre-operative consultation, we will thoroughly review your medical history, discuss your reasons for removal, and perform a physical examination. We’ll assess the current condition of your implants and breast tissue, and if a rupture is suspected, we may recommend an MRI or ultrasound. This is also your opportunity to discuss your aesthetic goals post-removal.
The surgery itself typically involves either intravenous (IV) sedation or general anesthesia, ensuring your comfort throughout the procedure. The surgical steps generally include making an incision, carefully removing the implants and any surrounding capsule or leaked silicone, and then closing the incisions.
After the implants and capsules are removed, we often send them for post-operative testing. This is particularly important if there were concerns about rupture, infection, or the presence of BIA-ALCL or SCC. Pathologists can examine the capsule tissue for abnormal cells, signs of inflammation, or malignancy (like CD30 testing for BIA-ALCL), and cultures can check for bacterial or fungal infections. This step provides valuable information for your ongoing health.
Preparing for Your Surgery
Preparing for your silicone implant removal surgery is key to a smooth experience and optimal recovery. We will provide you with specific instructions custom to your needs. Generally, these include:
- Medication Adjustments: You may need to adjust or temporarily stop certain medications, especially those that increase bleeding risks, such as anti-inflammatory drugs or certain herbal supplements.
- Stopping Smoking: If you smoke, we will strongly advise you to stop several weeks before surgery. Smoking can significantly impair healing and increase the risk of complications.
- Arranging for Post-Op Care: Since this is typically an outpatient procedure, you’ll need to arrange for a trusted friend or family member to drive you home and assist you during the initial recovery period.
- Dietary Guidelines: We may provide specific dietary guidelines for the days leading up to your surgery.
Choosing the right plastic surgeon is paramount for a successful silicone implant removal procedure. When you come in for your consultation in Scottsdale or Phoenix, we encourage you to ask us a comprehensive set of questions to ensure you feel confident and informed. Here’s a list of what to ask your surgeon:
- What is your experience with silicone implant removal and capsulectomy?
- How many implant removal procedures do you perform annually?
- What type of capsulectomy do you recommend for my situation (total, en bloc, partial) and why?
- What are the potential limitations in removing all capsule tissue or leaked silicone?
- What are your protocols for pathology and culture testing of removed tissue?
- Can I see before-and-after photos of your previous silicone implant removal patients?
- How do you address breast sagging or changes in breast shape after removal?
- What are the risks and potential complications of this specific surgery?
- What is the expected recovery timeline, and what kind of support will I receive?
- What is your approach to BII or autoimmune cases?
- What are my options for reconstruction or breast reshaping after removal?
- What is the total cost involved, and what does it include?
Surgical Techniques: Capsulectomy Explained
One of the most critical aspects of silicone implant removal is the management of the breast capsule—the scar tissue that naturally forms around the implant. The surgical removal of this capsule is called a capsulectomy, and there are different techniques, each with specific indications.
-
Implant Removal Only: In some cases, particularly with saline implants that have ruptured cleanly or if the capsule is very thin and healthy, only the implant may be removed, leaving the capsule intact. This is less common for silicone implants, especially if ruptured.
-
Partial Capsulectomy: This involves removing only a portion of the capsule. It might be performed if the capsule is adherent to vital structures, making complete removal risky, or if only a specific problematic area of the capsule needs to be addressed.
-
Total Capsulectomy: This technique involves removing the entire capsule after the implant has been taken out. The implant is typically removed first, and then the capsule is carefully dissected and removed in pieces. This is often indicated for grade 3 or 4 capsular contracture, or for intracapsular silicone ruptures where the gel is contained within the capsule.
-
En Bloc Capsulectomy: This is considered the most comprehensive technique. “En bloc” means “as a whole” or “in one piece.” During an en bloc capsulectomy, the implant and the entire surrounding capsule are removed together, without separating them. This approach is often preferred when there’s a concern about silicone leakage or biofilm contamination, as it aims to remove the implant and capsule contents completely intact. However, it is medically necessary only for the treatment of capsular malignancy, such as BIA-ALCL or SCC. While it can be performed for other reasons, it’s important to understand that its primary medical indication is malignancy. This technique can be more challenging and may not always be possible if the capsule is very thin, fragile, or densely adhered to surrounding tissues.
Choosing the right capsulectomy technique depends on your individual circumstances, the condition of your implants and capsule, and any medical concerns. We will discuss the most appropriate approach for your specific situation during your consultation, always prioritizing your safety and the best possible outcome.
For more information on breast revision procedures, including implant removal and replacement options, visit More info about Breast Revision.
Life After Explant: Recovery and Aesthetic Options
Life after silicone implant removal is a journey toward healing and refinding your natural contours. Understanding the recovery process and the potential aesthetic changes will help you prepare for this new chapter.
While silicone implant removal is generally a safe procedure, it’s important to be aware of potential risks and complications, similar to any surgery. These can include:
- Seroma: A collection of fluid under the skin, which may require drainage.
- Hematoma: A collection of blood under the skin, causing bruising and swelling.
- Infection: Though rare, infection is a possibility at the surgical site.
- Scarring: Incisions will result in scars, which typically fade over time but are permanent. We strive to place incisions discreetly.
- Asymmetry: Slight differences in breast shape or size may occur.
- Changes in Nipple Sensation: Some patients may experience temporary or permanent changes in nipple and breast sensation.
- Loose Skin: Depending on the size of the implants and skin elasticity, you may have loose skin after removal.
We will discuss all potential risks with you in detail during your consultation, ensuring you are fully informed.
Recovery After Silicone Implant Removal
The recovery period for silicone implant removal is generally manageable. You can typically expect an initial recovery phase of one to two weeks, with a full recovery taking approximately six weeks.
- Immediate Post-Op: After surgery, you’ll spend a couple of hours in a recovery room where your vital signs will be monitored. You may experience some mild pain and discomfort at the incision sites, which can be managed with prescribed pain medication.
- Drains: Small surgical drains might be placed to collect any excess fluid, typically for a few days to a week.
- Compression Garments: You will likely wear a special support bra or compression garment for several weeks to help reduce swelling, support your healing tissues, and ensure optimal shaping.
- Activity Restrictions: We will advise you to avoid strenuous activities, heavy lifting, and intense exercise for at least four to six weeks. Light walking is usually encouraged early on to promote circulation. You should also avoid driving for a few days post-surgery.
- Incision Care: We’ll provide detailed instructions on how to care for your incisions to promote healing and minimize scarring.
- When to Call Us: It’s crucial to contact our office immediately if you experience any signs of complications, such as chest pain, chills, fever, persistent or worsening pain, excessive swelling, or shortness of breath.
Most patients report that recovery from silicone implant removal is less extensive than their original augmentation, as the implant pocket is not being created or significantly expanded.
Restoring Your Breast Contour
A common question and concern for many women considering silicone implant removal is how their breasts will look afterward. It’s important to have realistic expectations. After implants are removed, it’s natural for your breasts to appear smaller, and some degree of sagging (ptosis), skin laxity, or volume loss may be present. This is especially true if you had large implants for many years, as the skin and tissues would have stretched to accommodate them.
However, if you’re concerned about sagging or a “deflated” appearance, there are excellent corrective options we can discuss to help restore your breast contour:
- Breast Lift (Mastopexy): This is a very popular procedure performed concurrently with silicone implant removal. A breast lift reshapes and repositions your breast tissue, removes excess skin, and lifts the nipple-areola complex to a more aesthetically pleasing position. This can significantly improve the shape and firmness of your breasts after implant removal.
- Fat Grafting: For those desiring a subtle increase in volume or to address minor contour irregularities, fat grafting (or autologous fat transfer) can be an option. This involves harvesting fat from another area of your body (like the abdomen or thighs) via liposuction, processing it, and then injecting it into your breasts. This uses your body’s own tissue to add volume and improve shape naturally.
We will work with you to understand your goals and recommend the best approach to achieve a satisfying aesthetic result following your silicone implant removal in Scottsdale or Phoenix.
For those interested in combining implant removal with a lift to achieve a more youthful and uplifted appearance, you can find more information here: More info about Breast Augmentation with Lift.
Frequently Asked Questions about Implant Removal
We understand you have many questions about silicone implant removal, and we’re here to provide clear, comprehensive answers.
How much does silicone implant removal cost?
The average cost of breast implant removal can be several thousand dollars, but this is a highly variable figure. According to the American Society of Plastic Surgeons (ASPS), the average cost can vary significantly. The total cost of your silicone implant removal will depend on several factors:
- Surgeon’s Fee: This is based on the surgeon’s experience, reputation, and the complexity of your case (e.g., whether a capsulectomy or a breast lift is performed).
- Anesthesia Fees: These costs are determined by the type of anesthesia used and the duration of the surgery.
- Facility Fees: These cover the use of the surgical facility.
- Other Related Expenses: This can include pre-operative tests, post-operative garments, and prescription medications.
Insurance Coverage: This is a common and often complex question. Insurance coverage for silicone implant removal typically depends on whether the procedure is deemed medically necessary versus purely cosmetic.
- Medical Necessity: If your implant removal is due to complications such as rupture, severe capsular contracture (Baker Class III or IV with pain), BIA-ALCL, recurrent infections, or interference with mammography, it is often considered medically necessary. In such cases, insurance may cover a significant portion of the cost. The Women’s Health and Cancer Rights Act (WHCRA) of 1998 may require coverage if the initial mastectomy was medically necessary. When discussing medical necessity with your insurance, focusing on functional issues (pain, limited motion, confirmed rupture) rather than just “Breast Implant Illness” symptoms can often be more effective, as BII is not yet a universally recognized diagnosis by all insurance providers.
- Cosmetic Reasons: If you are removing your implants purely due to a change in aesthetic preference or dissatisfaction without a medical complication, it will likely be considered a cosmetic procedure and not covered by insurance. If you choose to have a breast lift or fat grafting concurrently for aesthetic improvement, these elements are typically not covered by insurance.
We will work with you to provide the necessary documentation for your insurance company if your silicone implant removal is medically indicated. For more detailed information on costs, you can consult resources like the ASPS data on removal costs.
Will my breasts look “deflated” after removal?
This is one of the most frequently asked questions, and it’s a very valid concern! Yes, some degree of volume loss and potentially sagging is expected after silicone implant removal. Your breasts will naturally look smaller without the implants. The extent of this change largely depends on:
- Original Implant Size: Larger implants tend to stretch the skin more, leading to more noticeable laxity after removal.
- Skin Elasticity: Younger patients or those with good skin elasticity may experience less sagging.
- Time with Implants: The longer you’ve had implants, the more stretched your tissues may be.
- Natural Breast Tissue: The amount of natural breast tissue you have will also influence the post-explant appearance.
While your breasts may not return to their pre-augmentation shape, many people opt for a breast lift (mastopexy) concurrently with their silicone implant removal. This procedure can remove excess skin, tighten the remaining tissue, and reshape the breast to create a more lifted and aesthetically pleasing contour. We can discuss these options in detail to help you achieve the best possible result.
How do I find a surgeon experienced in explant surgery?
Choosing the right surgeon for your silicone implant removal is paramount, especially given the nuances of capsulectomy and potential complications. Here are the key factors to consider:
- Board-Certification is Key: Always choose a plastic surgeon who is board-certified by the American Board of Plastic Surgery. This ensures they have met rigorous standards for training, experience, and ethical practice.
- Look for Experience in Breast Revision and Explant: Seek a surgeon with specific, experience in breast implant removal and breast revision surgeries. Don’t hesitate to ask about their volume of explant cases.
- Review Before-and-After Photos: A surgeon’s gallery of before-and-after photos can provide valuable insight into their aesthetic style and the results they achieve for patients undergoing silicone implant removal, especially those including breast lifts.
- Choose a Surgeon Who Listens to Your Goals: A good surgeon will take the time to listen to your concerns, understand your motivations for removal, and discuss your aesthetic goals thoroughly. They should clearly explain the procedure, potential outcomes, and all associated risks.
- Transparency and Communication: Ensure the surgeon is transparent about their recommended surgical technique (e.g., total vs. en bloc capsulectomy), potential limitations, and post-operative care.
In Scottsdale, Dr. Malek is known for his personalized approach and expertise in breast surgery, including silicone implant removal. We invite you to Contact Dr. Malek for a consultation to discuss your needs.
Your Next Step Towards a Renewed You
Deciding on silicone implant removal is a significant personal journey, often involving careful consideration of your health, well-being, and aesthetic desires. We hope this guide has provided you with a clear understanding of the procedure, why it might be necessary, what to expect, and the options available to you for a renewed sense of self.
Our goal is to empower you with informed choices. Whether your decision is driven by medical necessity, a change in lifestyle, or simply a desire to accept your natural beauty, we are here to support you every step of the way. Dr. Malek’s artistic and patient-focused approach in Scottsdale ensures that your experience is as comfortable and personalized as possible, with a commitment to delivering fantastic, long-lasting results.
Taking the first step is often the hardest, but it’s also the most crucial. If you are considering silicone implant removal or breast revision, we encourage you to reach out.
Schedule your breast revision consultation today to discuss your unique situation and explore how we can help you achieve your personal goals.